DAVID KIRBY INTERVIEW WITH TOM INSEL*
December 18, 2009
DK: I would like to get your interpretation of the new autism numbers out today. Even the CDC said that "We cannot rule out" an actual increase in the risk for autism. So if better reporting, awareness and diagnosis cannot account for all the increase, what else do you think might explain it?
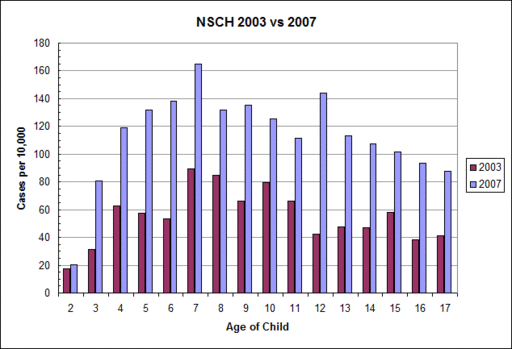
TI: It's the question that everybody's asking. I would point you to three sources for information on questions of prevalence. There is HRSA, which has done phone surveys. There is CDC, which has been using basically the same methodology across all of these different cohorts focusing just on 8 year olds and using secondary data sources. And the third source is the California registry, the DDS data, which goes back to 1987 and has data from every year on children who were referred in for services. In which case, because it is a disability services registry, you are talking about children who are on the more severe end of the autism spectrum. And as far as we know, they are not actually seeing the kids who might be called Aspergers, or on the more functional end.*
So the interesting thing about this is, from the California data we actually have a chance to investigate this question of how much of this is a real increase, and how much of it can be explained away by ascertainment, by changes in diagnosis, and by all of these other issues. And I think right now, based on what we are seeing from the California data, is that it's not really a question about whether this increase is real or not. The question is, how much of it can be attributed to each of the many factors that one might be interested in.*
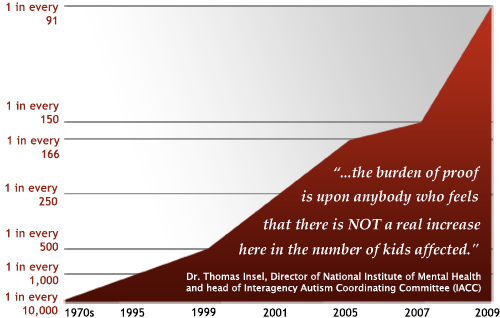
So how much of the doubling or - in this case tenfold increase over a decade - how much of it is related to change in diagnosis, how much to ascertainment? It looks like about 24 percent of the California increase can be attributed to something like a change in diagnosis criteria. They are beginning to use multiple diagnoses. So that children before, who were listed simply as mentally retarded rather than autism - but they had both - are now logged in with both. But that really caps out at around 24 percent. There's probably another piece of this, which globally could be attributed to ascertainment. But that caps out at around 16 percent, or something like that. And when you put all of that together, you are still well below explaining 50 percent of the increase.
So what does that mean? It means that, as far as I can tell, the burden of proof is upon anybody who feels that there is NOT a real increase here in the number of kids affected. Because all of the evidence we have up until now says that, well there are what we could call – I wouldn't call them 'trivial' factors – but they are factors that are not related to incidence, but would be simply related to prevalence, like ascertainment. But they don't really explain away this huge increase.*
This tells you that, you really have to take this very seriously. From everything they are looking at, this is not something that can be explained away by methodology, by diagnosis. Some piece of it can, but the whole thing can't.*
DK: So that leads to the 64 million dollar question: If there is an actual increase in incidence year to year, wouldn't there necessarily also have to be an environmental component to at least some cases of autism? In other words, if it was 100-percent genetic, wouldn't you see relative stability?
TI: Yes. I don't think anybody is arguing that it is 100-percent genetic. I mean, I think that there are just a lot of questions that this raises. And I don't think in those terms, exactly, that it's either genetic or it's environmental. From my perspective, it's almost always going to be both. And the only question is: How do you nail down this interaction, how do you go after it?
DK: If there is a true increase, wouldn't that be due to environmental factors rather than genetic factors?*
TI: I don't know that anybody would argue that, or that anybody has argued that. There is no question that there has got to be an environmental component here. The problem for us has been trying to find the right way to get our hands around it, and to identify what that is most likely related to. *
I think, if you look at whatever that factor is, the way we tend to do this in medicine is that you look for geographic clusters or temporal clusters. And I don't think we have… we have a few, but there are not very many good geographic clusters. It could be that the Somali story in Minneapolis is an important geographic cluster. It could be that there are clusters that have actually been indentified in California. It's a little too early - and I don't think the data are published – but I have seen some data in unpublished form that would suggest that that may turn out to be the case. These are new data, from work by Peter Bierman, who is an NIH Pioneer Awardee. He's at Columbia.
DK: Can you tell me where those clusters are in California?
TI: I don't actually know enough of the details. He presented his work here about two months ago. So I can't tell you exactly where they are, but I can tell you that they exist. And again, the explanation for that is not clear.
DK: Are you familiar with the Minnesota study of the Superfund sites and the increased rate of ASDs in proximity to those sites?
TI: I don't know that. Where were those data published?
DK: I can get it for you, it was definitely peer reviewed. I don't have it right at my fingertips, but it was a fairly recent study.
TI: You know, we have this stuff - I think it is from the CHARGE study - that looked at organophosphate fertilizers in California and exposures in the second trimester. I don't know if you've seen that.
DK: I've seen the pesticide study from the Central Valley.
TI: Yes, the pesticide study. And, I mean, it's pretty clear there's a signal there. So, again, I don't think anyone argues the fact that there's an environmental component here. The question is – there may be many, and how do we get at these, and how do we identify them? Because the real goal here is to think about prevention – what we are really after at this point is driving the numbers in the opposite direction, so instead of a tenfold increase, you can we see a tenfold decrease.
DK: And you think that is possible?
TI: I think that, if you could identify the factors that are really pushing this, then I think you can begin to bend the curve. Here's the issue for me, and I think I am arguing, probably, against the wave of the people that are in this field. But I think that we're approaching autism as if it is a single thing, as if it is a syndrome that will have one cause, one treatment, and one explanation. I tend to think of it more in the way we think of fever. I think this is a collection of many, many different disorders. And part of the reason why you see so much polarization in the community is because there is a tendency for people to think that their experience is the same as everybody else with a child with autism.
It's quite believable to me that there are many children who develop autism in the context of having severe gut pathology, of having autoimmune problems, of having lots of other problems. And some of these kids really do recover. And that is quite different from the autism that was originally described in the 1940s and 50s - where it looks like you have it and you are going to have it for the rest of your life. And at that point, it's a disorder that is mostly manifest by these huge social deficits.*
So I don't know if what we have here are 10 different disorders or 20 different disorders. What I think hangs up this field is the inability to indentify all these different autisms – and it's very much where we were with infectious disease 100 years ago, before we knew how to break this down into multiple different disorders, different causes, different treatments. That's why fever seems like the right analogy. In this context, I don't think anyone would be able to argue very strongly that there is not some subgroup that's going to be unrelated to genetics -- like those kids who have Fragile X -- and some subgroups that may be much cleaner on the genetic side, but will have some environmental exposure that triggers the disorder.
DK: And probably a genetic susceptibility?
TI: That hasn't been tracked down yet. But this is the cool thing and, I think, something that many in the community don't understand. And that is, in the last few months, or maybe year, we've begun to develop the tools that will allow us to get at this. And these tools are from this whole emerging field of epigenetics, or epigenomics. And in this case you are not looking at genetic sequence - which is what we've been doing for the last decade - but you're looking at how the DNA is bound up with all kinds of proteins. That is largely affected by experience, or by environment. Some of it is probably hardwired, but a lot of it has to do with exposures, particularly early in development but even, as we are learning, even after birth*
So what we are really excited about here, I think, is to be able to use these new tools. And what has only happened in the last month or two is the first whole genome epigenetics effort, where we have been able to say, 'We can map this entire aspect of genomic biology, and it tells us what someone's exposure history might have been.' It shows you effectively, or we are hoping it will show us, where the scars might be from early exposures.
DK: Like a footprint?
TI: Precisely. And if that works, that would be a way in which, finally, we would have the technology that says, 'Ah, this is somebody who was exposed to organophosphates, or perhaps to some infection, or some autoimmune process, or something like that, that could really make a difference in the way the brain is developing.' And now they are signaling that I have to get off this call.
DK: That's wonderful news. Let me ask you just a few quick questions more, because I want to make sure I am clear. Let me ask you your personal opinion: Is there an actual increase and is there an environmental component to it?*
TI: My personal sense, just from my clinical experience… when I was in training, I never saw a child with autism. So I went through four years of training as a psychiatrist, including a rotation – a long one – through a year of child psychiatry, and never saw a case. I got interested in autism through work I was doing in basic science research, and I wanted to see children with autism. I couldn't find them. This was in the mid-1980s, and I had to find a specialty clinic at Children's Hospital in Washington, and I got to see my first case there. And now I wouldn't have to go any further than the block where I live to see kids with autism today. So if that's not a change, I don't know what is. On a personal experience basis, I don't think that's unusual. Most people who I've trained with would say much the same thing. So, of course, I think all of us are much more aware of autism than we would have been 20 years ago. And again, I want to stress, I don't think it's just a difference in awareness, I think that there is something that we need to get our hands around here.
DK: Have you looked into the XMRV connection at all?
TI: Yeah, last thing. We are hot on that, and I wish I could tell you more. All I can tell you is that we have an intramural program here which is kind of our home team, which has seen about 400 kid with autism over the last couple of years. And they have been looking at regression; they've been looking at recovery. They are very interested in a lot of the exciting parts of this story – they jumped on the XMRV thing even before it was published. I don't know how they got news about this, but they had already found someone who could start to look into this.
DK: Dr. Mikovits?
TI: No, they were working with someone through the National Institute of Allergy and Infectious Disease, who apparently had antibodies. And they sent off serum, and I think they sent off CSF, cerebral-spinal fluid, one day after the presentation. And I haven't seen the results, but they are really hot on the trail here to see if there is any story. I've heard that there is something coming out from the group in Nevada, but I haven't seen the data. Have you seen it?
DK: No. She announced on television that, in a small sample of ASD kids, they found it in 40 percent.*
TI: Yeah, that's the number I got. I have been trying to track that. There is a paper that has been submitted, but I haven't been able to get it, and I don't know what the data look like. But I think this is really interesting.
DK: I also understand a number of the Vaccine Court Omnibus cases are now vigorously testing and finding it to be quite common. And there are rumors that the parents are testing negative. Now, that's just a rumor, I can't confirm it, but that would be an interesting development.
TI: So, of course, if we could just find a small group, and the opportunity to begin an antiretroviral treatment regime, that could be terrific, wouldn't it? I mean, that would be the kind of thing we're really looking for in this field, is finding the subgroups that might have specific therapies that would make a difference. And that's what we're missing. I mean, frankly, we're just not where we want to be yet, and we've got to be able to break apart this spectrum disorder into its component parts and identify who's going to respond to which interventions.*
DK Finally, I know you have to go, will IACC reconsider vaccine research and -- given this new data -- in particular Hepatitis B coverage? Because that is something that changed significantly between 94 and 98.
TI: I don't know what they will do. You know, I chair the committee, but I let them bring issues up. I am open to whatever they want. As you know, what happened with the whole idea of having vaccine studies earlier in the year was a majority vote. And, I think what you are going to see with this update is that there is a recognition that we need to look at subgroups who might be particularly responsive to environmental factors. And, you know, at the end of the day, the IACC will have some sort of guide on what they hope to have funded. But it's going to be up to the institutes, and the CDC, to actually do the funding.
DK: Well, what is your opinion, or your response to the fact that in 1994 the Hep B birth dose was around 27 percent coverage, and by 1998 it was above 90, I believe?*
TI: Yeah, I don't know what to do with that, but I have to sign off here. Maybe we can start there with our next conversation?
DK: OK great. I look forward to it in the New Year.
TI: Great. I look forward to talking with you then.